AI Eligibility & Benefits
Autonomous eligibility verification and contextual benefit interpretation — delivered in real time.
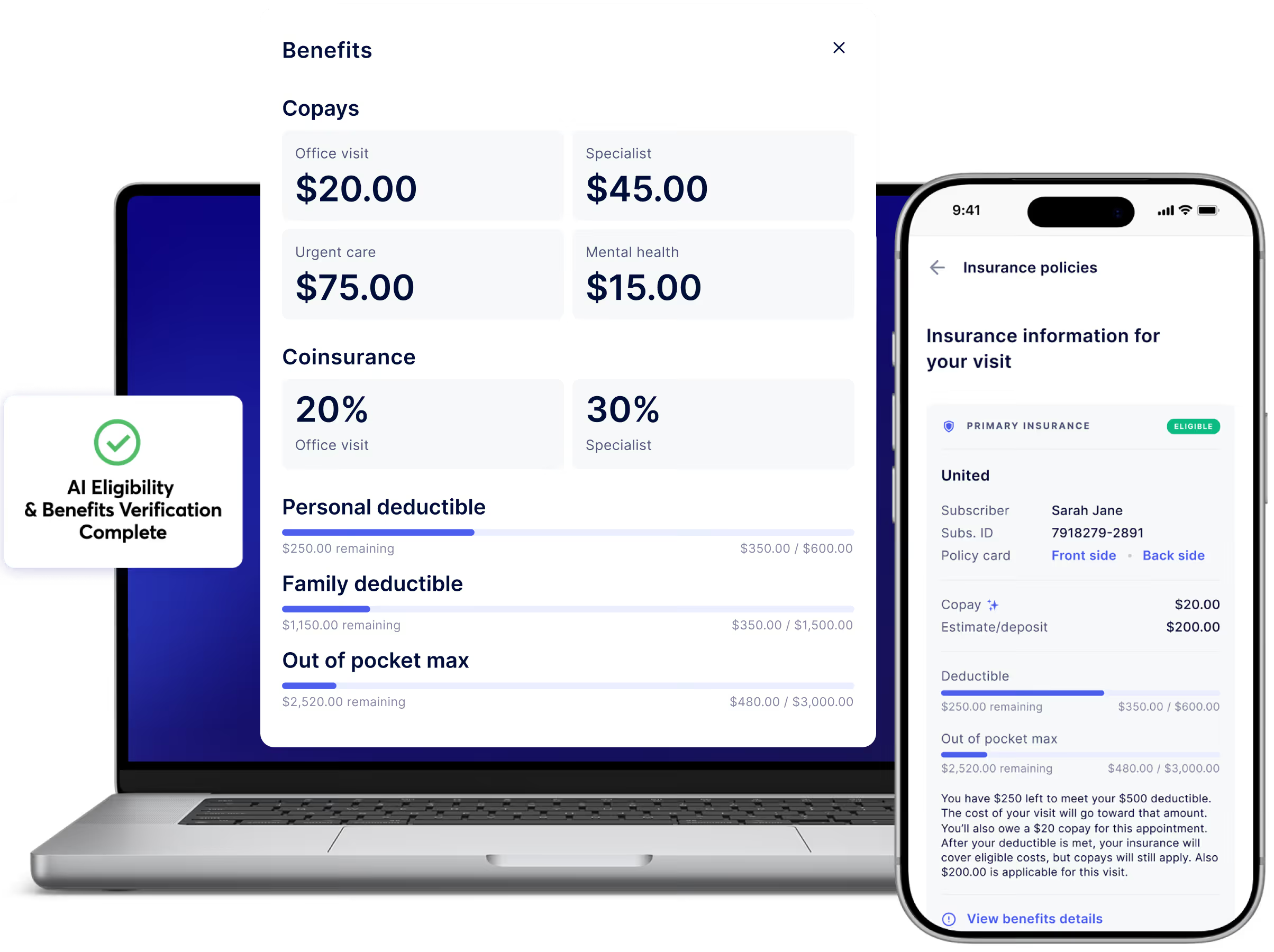
Collectly's Billie AI agent retrieves benefits data from clearinghouses and payer portals, then interprets coverage to surface actionable patient financial details like copays, deductibles, and responsibility.
What once took 12–15 minutes per patient now happens in seconds — with human review only when needed.
Automation Rate
Payer Access Coverage
First-Pass Accuracy Improvement
Per Patient
Eligibility and benefits remain one of the most manual, error-prone steps in healthcare finance
See How Collectly Transforms Your Workflow
Before
After
Beyond Verification: Context-Aware Interpretation
Traditional systems return raw 271 data or require manual portal review. Collectly surfaces structured, appointment-aware financial details automatically — so staff and patients see clear, usable information instead of payer code fragments.
Copays, deductibles, coinsurance, carve-outs, secondary coverage, and prior authorization requirements are extracted and organized in real time — eliminating manual interpretation and reducing surprises before care is delivered.
Intelligent Eligibility & Benefits Capabilities
Automated Payer Portal Access & Retrieval
Securely accesses payer portals to retrieve complete benefits data beyond standard EDI — including plan documents, benefit summaries, and secondary coverage.
Autonomous Eligibility Verification
AI agent autonomously verifies coverage across payers in real time — eliminating manual portal logins, phone calls, and repetitive verification tasks.
Context-Aware Benefit Interpretation
Interprets benefits in clinical context using CPT, ICD, and appointment data — delivering actionable financial information, not raw eligibility responses.
LLM-Driven 271 Analysis
Applies large language model reasoning to parse and interpret complex 271 responses — extracting copays, deductibles, coinsurance, and carve-outs with high confidence.
Secondary & Carve-Out Detection
Automatically identifies secondary insurance, tertiary coverage, and benefit carve-outs — preventing downstream denials and billing surprises.
Appointment-Aware Copay Determination
Applies benefit rules to scheduled procedures and visit types to surface accurate copay and responsibility information before care is delivered.
Related Products
These products work great together with AI Eligibility & Benefits

See AI Eligibility & Benefits in Action
Learn how Collectly can transform your pre-visit operations.