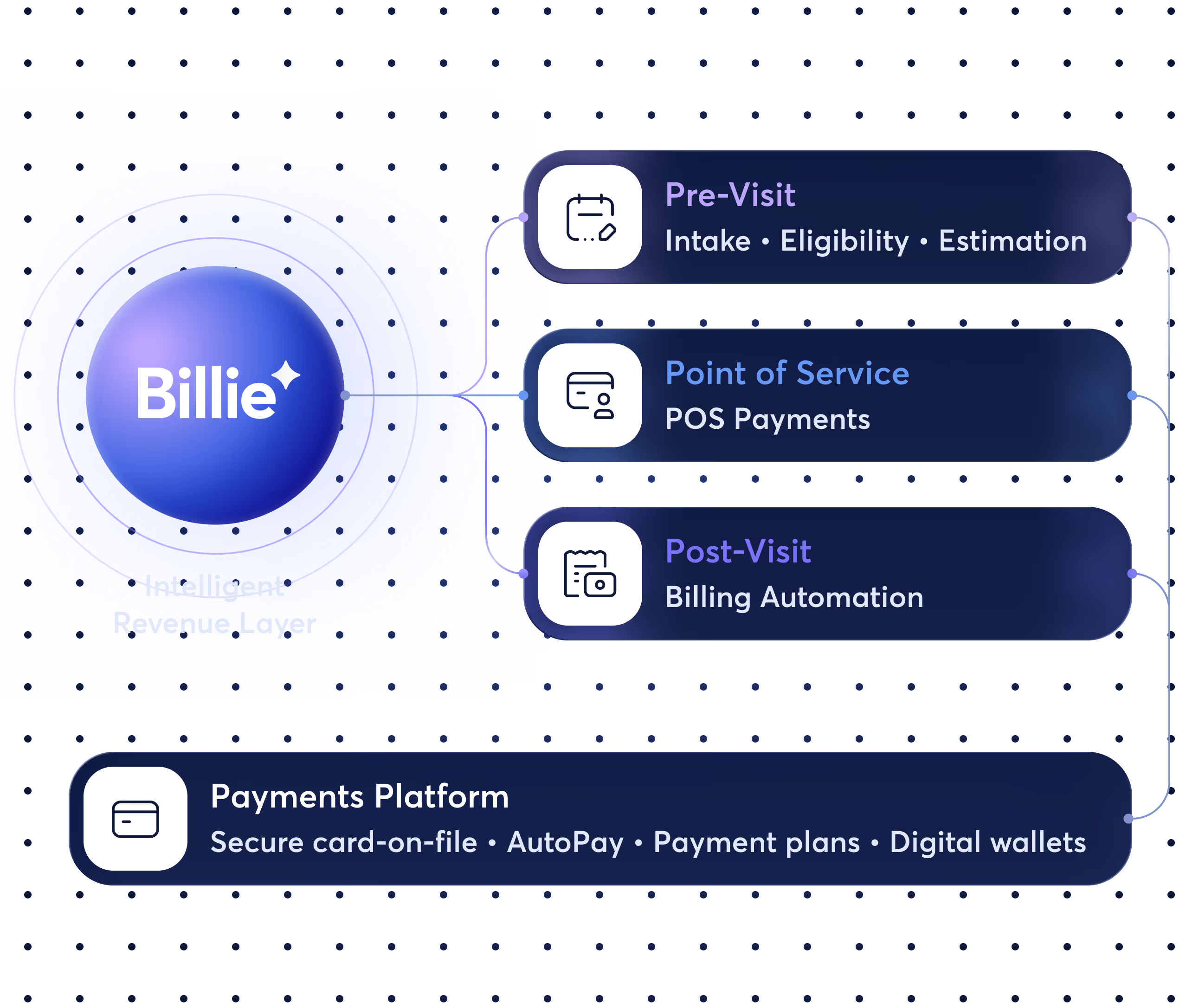
Pre-Visit Intake Automation
Digitize patient intake so registration, consent, and pre-service payment requests happen before patients arrive — reducing check-in time, preventing errors, and improving front desk throughput.
AI Eligibility & Benefits
Automate eligibility and benefits verification with real-time results — interpreting payer responses into visit-specific coverage details so teams stop relying on portals, guesswork, and manual review.
AI Cost Estimation
Predict patient responsibility before care using AI-powered estimation — improving financial transparency, reducing surprise bills, and increasing pre-service collections.
Point-of-Service Payments
Capture copays and balances at the front desk with integrated checkout workflows and modern payment hardware — including terminals and iPad experiences — synced to the EHR to prevent reconciliation gaps and downstream A/R.
Post-Visit Billing Automation
Automate the post-visit billing cycle with digital statements, smart reminders, and AI-powered support — so patients resolve balances faster and teams reduce time spent on repetitive billing work.
Payments Platform
A unified payments infrastructure that powers the entire revenue cycle — from pre-service card capture and payment requests, to point-of-service checkout, to post-visit payment plans and reconciliation.
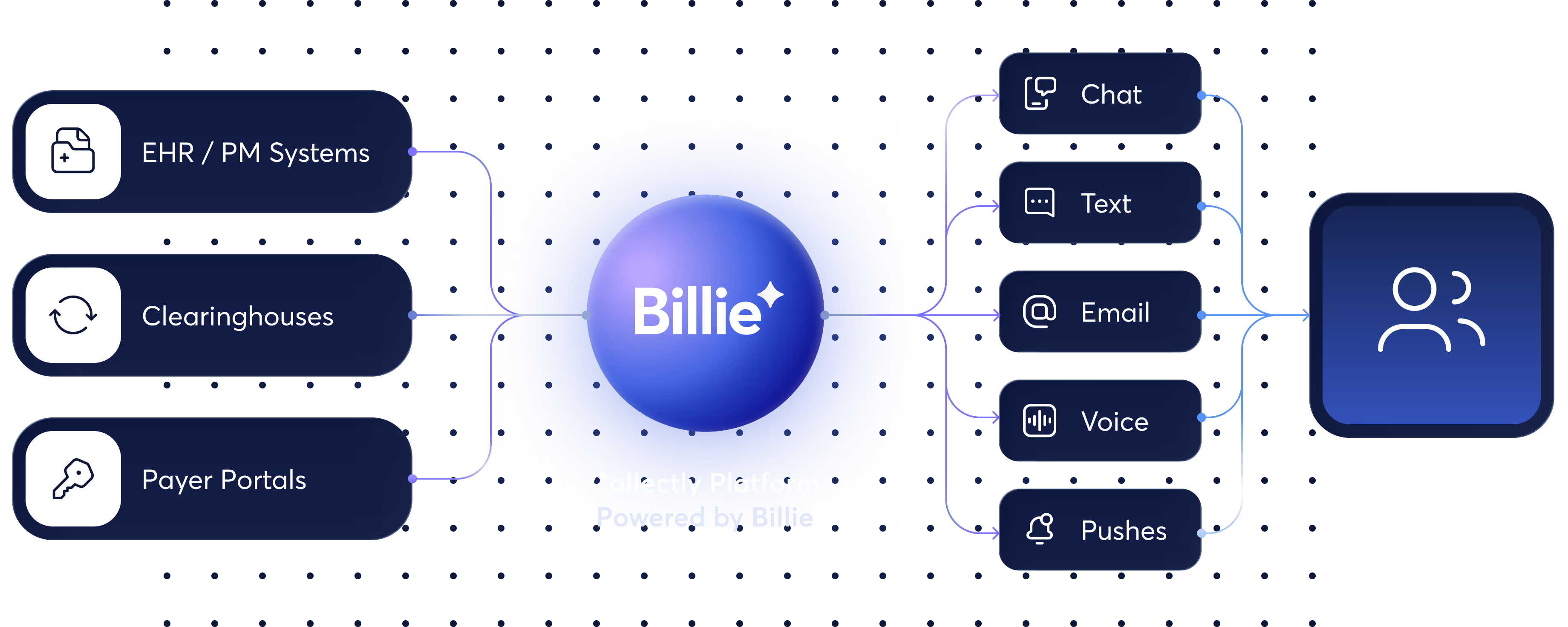
Built to Integrate With Your Revenue Cycle — Not Replace It
The Collectly platform integrates into your existing ecosystem — powered by Billie to connect systems, workflows, and patient communication channels across your revenue cycle.